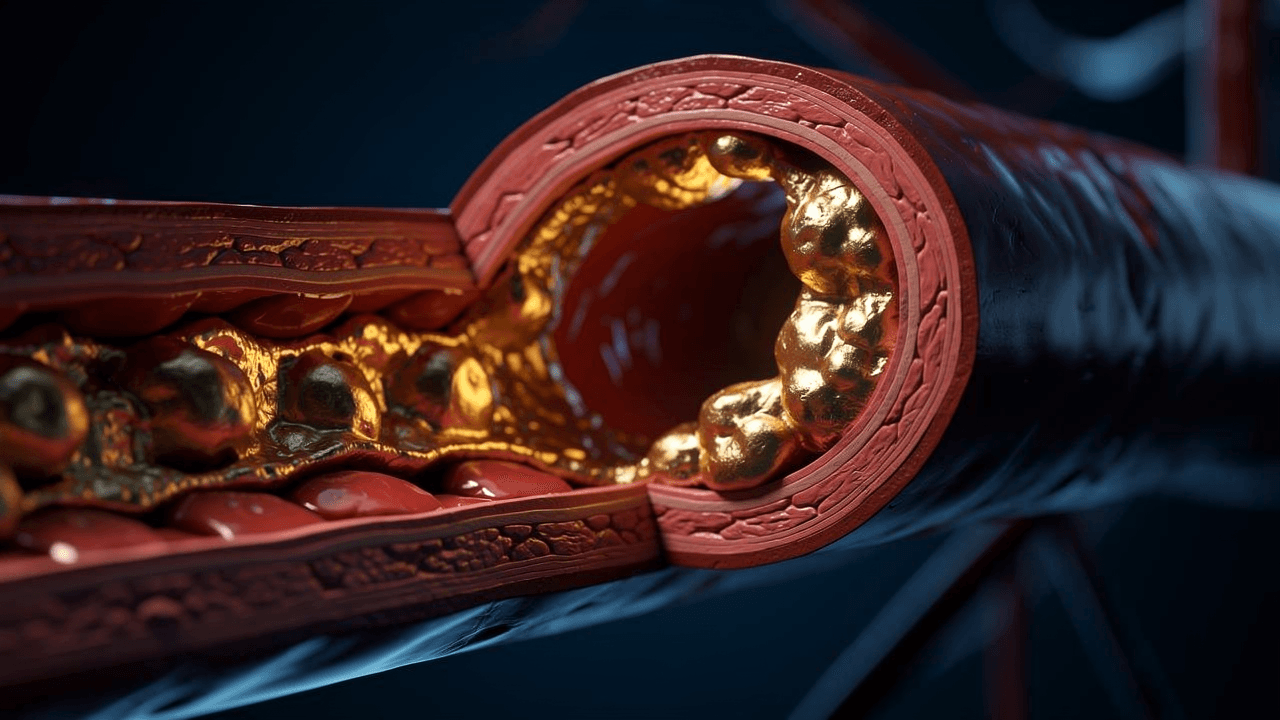
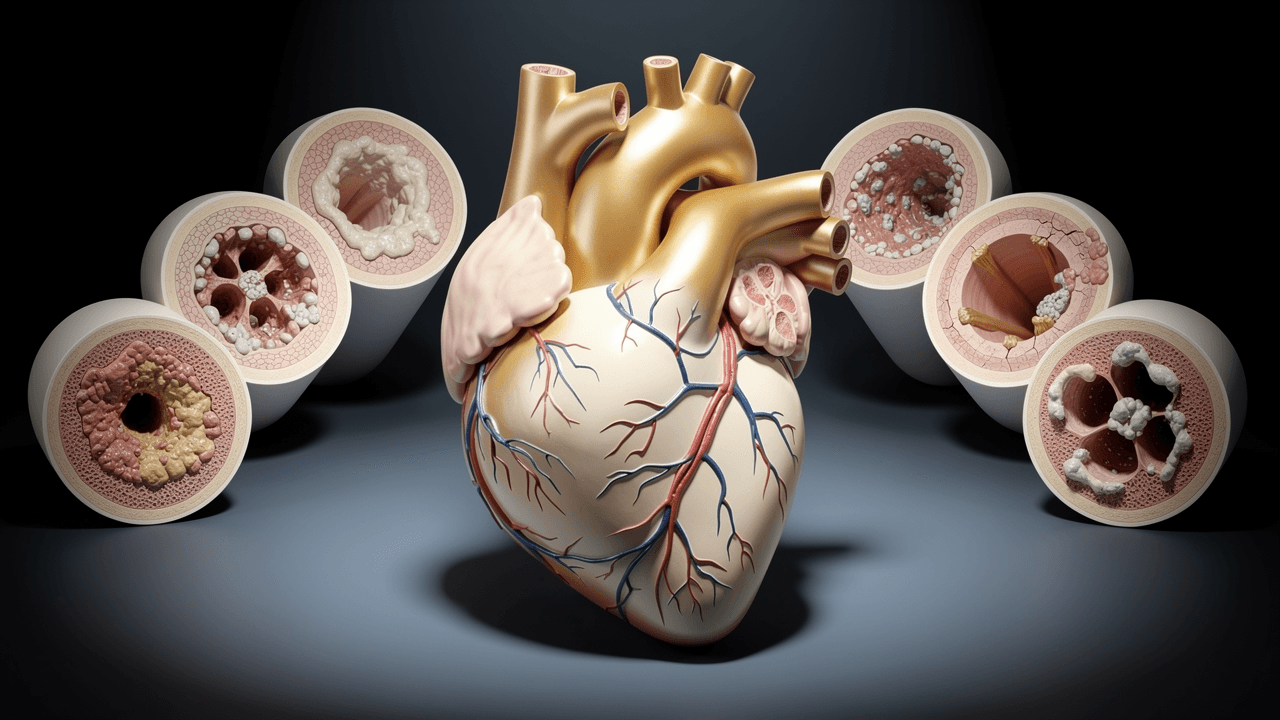
Roughly 1 in 5 people in the UK carries a genetically elevated Lipoprotein(a), a modified cholesterol particle that is up to seven times more atherogenic than ordinary LDL and that virtually no GP measures as part of routine care. A further large group has a pattern of elevated atherogenic particle burden visible only through ApoB, not the standard LDL-C calculation. And many of those same patients have impaired clearance of triglyceride-rich remnant particles, a third pathway that silently accelerates plaque growth in the arterial wall throughout the day.
The clinical problem is not simply that these markers are unmeasured. It is that they are three mechanistically distinct routes to the same destination, atherosclerotic cardiovascular disease, and they can compound each other's effect. Having all three elevated is not the same as multiplying three individual risks. The biology overlaps, reinforces, and in some cases amplifies.
Clinical bottom line: a normal NHS cholesterol result does not exclude three of the most important drivers of preventable cardiovascular disease. Without Lp(a), ApoB, and an assessment of triglyceride-rich lipoprotein burden, the picture is incomplete.
Why your standard cholesterol test leaves three major risk pathways unmeasured
The NHS standard lipid panel has not fundamentally changed in decades: total cholesterol, LDL-C (usually calculated using the Friedewald equation), HDL-C, triglycerides, and the TC/HDL ratio. This panel was designed to be cheap, widely available, and practically useful at a population level, and for those goals it is adequate.
But it was not designed to detect early individual-level cardiovascular risk in people who are metabolically stressed, genetically predisposed, or who want to act before plaque is established. For that purpose, three categories of information are systematically missing:
- The number of atherogenic particles in circulation (ApoB), as distinct from the cholesterol they carry.
- The presence and level of Lipoprotein(a), a genetically determined particle that drives atherogenesis, thrombosis, and aortic valve calcification through mechanisms completely separate from LDL.
- The clearance efficiency of triglyceride-rich lipoprotein remnants, small, cholesterol-laden particles that can enter the arterial wall directly and are far more atherogenic per-particle than large VLDL.
The 2023 ESC/EAS Dyslipidaemia Guidelines (updated again in 2025) now explicitly classify Lp(a) as an independent cardiovascular risk factor, not a modifier, not a footnote. The 2026 ACC/AHA Dyslipidaemia Guideline (published late 2025) places both ApoB and Lp(a) alongside LDL-C as markers warranting clinical action. UK practice has not yet caught up to these guideline changes at a primary care level, which means the gap between what science recommends and what most patients are offered is widening.
Lipoprotein(a): the genetically fixed risk that 1 in 5 people carry, usually without knowing
Lipoprotein(a), written Lp(a) and pronounced "L-P-little-a," is structurally similar to an LDL particle, but with an additional protein called apolipoprotein(a) [apo(a)] covalently attached. That structural difference changes everything about how it behaves in the body.
Apo(a) is molecularly similar to plasminogen, the body's primary clot-dissolving protein. This means Lp(a) does not just deposit cholesterol into arterial plaques like ordinary LDL. It also interferes with the body's ability to dissolve clots (antifibrinolytic effect), carries oxidised phospholipids that directly drive vascular inflammation, and accumulates in heart valves, promoting the calcification that eventually leads to aortic stenosis. It is, per particle, estimated to be five to seven times more atherogenic than LDL-C at equivalent concentrations.
What the data shows: At extreme Lp(a) levels above 300 nmol/L, the hazard ratio for myocardial infarction reaches 3.6–3.7 compared to those with minimal Lp(a). Even in statin-treated patients who have "achieved" their LDL-C goal, an Lp(a) above 50 mg/dL is associated with a 38–90% higher residual ASCVD risk depending on concurrent LDL burden (Circulation, 2024 meta-analysis).
Lp(a) is 70–90% genetically determined. It is, in practical terms, inherited, and it needs to be measured only once in adult life (in the absence of significant clinical change). Lifestyle changes have minimal impact. A plant-based diet, paradoxically, may modestly raise Lp(a) in some people. Statins do not lower it and may marginally raise it. PCSK9 inhibitors reduce it by around 25%, which is meaningful but insufficient for very high levels.
The reference range context matters greatly in the UK. Most standard NHS labs that do measure Lp(a) at all report in mg/L mass units, a different scale entirely from the nmol/L units used in the ESC/EAS guidelines. The ESC/EAS define elevated Lp(a) as above 105 nmol/L (approximately 50 mg/dL). The NHS "normal" range, where reported at all, is often quoted as below 300 mg/L, a completely different assay with no fixed conversion ratio. Patients reading their own results across different labs are frequently misled.
Ethnicity matters significantly. UK Biobank data shows median Lp(a) of approximately 19 nmol/L in White British adults, 31 nmol/L in South Asian adults, and 75 nmol/L in Black African or Caribbean adults, with many individuals in the last group reaching levels above 200 nmol/L. Black African and Caribbean patients in the UK carry disproportionately high Lp(a) burden and are simultaneously among the least likely to be tested.
A transformative pharmacological pipeline is approaching, but it is not yet available for clinical use. Phase 3 trials of RNA-based therapies, including pelacarsen (Novartis), olpasiran (Amgen), zerlasiran (Silence Therapeutics), and the oral agent muvalaplin (AstraZeneca/Ionis), are collectively expected to reduce Lp(a) by 80–90%. Readouts are anticipated between 2025 and 2028. If cardiovascular event reduction tracks the predicted 25–40% reduction, it will reshape preventive cardiology. For patients today, this means knowing your Lp(a) has immediate management implications: it changes risk stratification, informs decisions about PCSK9 inhibitors, drives more aggressive LDL-C targets, and may inform discussions about coronary artery calcium scoring.
ApoB: the particle count that reveals what LDL-C often hides
Every atherogenic lipoprotein particle, including every VLDL, every IDL, every LDL, every small dense LDL, and every Lp(a), carries exactly one molecule of ApoB. This makes ApoB a direct count of atherogenic particle traffic through the bloodstream. One particle, one ApoB. There are no exceptions.
LDL-C measures the total cholesterol content inside LDL particles. If those particles are large and cholesterol-rich, LDL-C is a reasonable proxy for particle number. But if the particles are small, dense, and individually cholesterol-depleted, which is exactly what happens in insulin resistance, metabolic syndrome, hypertriglyceridaemia, and fatty liver, then LDL-C substantially underestimates particle number. A patient can have an LDL-C of 2.8 mmol/L and an ApoB equivalent to someone with LDL-C of 4.5 mmol/L in good metabolic health.
The 2024 European Heart Journal analysis (Waldeyer et al., n>40,000) quantified this gap: in patients with elevated triglycerides, nearly 40% had discordantly elevated ApoB despite LDL-C appearing within normal limits. This is the clinical population most at risk of false reassurance from a standard lipid panel, and it is a very large population in the UK given the prevalence of metabolic dysfunction.
The 2026 ACC/AHA Dyslipidaemia Guideline now assigns ApoB explicit treatment targets: below 90 mg/dL for intermediate risk, below 70 mg/dL for high risk, and below 60 mg/dL for patients with established cardiovascular disease. The NLA 2024 Expert Consensus aligns with these numbers. These targets are substantially lower than the "laboratory normal" reference of below 130 mg/dL that most UK labs print on results. A patient at 95 mg/dL may be told their ApoB is "normal" when the current evidence suggests that for a 45-year-old with risk factors, it is not optimal.
Triglyceride-rich remnant particles: the third pathway working between your meals
Fasting triglycerides are the commonest measure reported on a lipid panel, but they are an incomplete window into the triglyceride story. The more atherogenic actors are the triglyceride-rich lipoprotein (TRL) remnant particles, partially metabolised VLDL and chylomicron remnants that circulate at elevated levels throughout the day, particularly in the hours after eating.
Unlike large VLDL particles, TRL remnants are small enough to enter the arterial intima, and unlike LDL, they do not require oxidative modification to be taken up by macrophages. They are directly and acutely atherogenic in the arterial wall. The Copenhagen City Heart Study data demonstrated that for every 1 mmol/L increase in remnant cholesterol (the cholesterol content of TRL remnants, calculated as total cholesterol minus LDL-C minus HDL-C), coronary heart disease risk increases by 2.8-fold, a larger effect size than the equivalent LDL-C increment.
The mechanism connects directly to the ApoB picture. In insulin-resistant individuals, the liver's VLDL production is not properly suppressed between meals. The liver keeps overproducing VLDL particles, flooding the system. Cholesterol ester transfer protein (CETP) then exchanges triglycerides from these VLDL particles into LDL and HDL, creating the classic dyslipidaemia pattern: high triglycerides, low HDL, and a shift towards smaller, denser LDL particles with higher particle numbers and elevated ApoB. The three markers are not merely co-existing. In metabolic dysfunction, they are mechanistically linked.
Key insight on timing: a 2025 study in Atherosclerosis confirmed that elevated triglycerides predict residual cardiovascular events and mortality independent of lipid targets and lipid-lowering therapy intensity , meaning patients on statins who have "hit" their LDL-C goal continue to have elevated event rates if their TRL clearance is impaired. Triglycerides are not just a risk marker. They are an active atherogenic mechanism.
What drives pathological TRL accumulation? Insulin resistance, MASLD (metabolic-associated steatotic liver disease, formerly NAFLD), excess visceral fat, sedentary lifestyle, high refined carbohydrate intake, and alcohol consumption. Critically, fasting triglycerides can appear in the "acceptable" NHS range (1.5–2.0 mmol/L) while postprandial TRL clearance is severely impaired; a patient can look fine on a standard panel while experiencing significant postprandial atherogenic exposure for six to eight hours after each meal.
The optimal fasting triglyceride in a longevity context is below 1.0 mmol/L, not the NHS flag threshold of 1.7 mmol/L. Levels between 1.0 and 1.7 mmol/L represent a borderline state that warrants attention even if no standard alert is triggered.
When all three are elevated simultaneously: why the risk compounds rather than simply adds
The clinically important question is not just whether each marker is elevated in isolation, but what happens when all three are present together. The answer from the research is that the risk is substantially greater than additive, approaching multiplicative, for two reasons.
First, these are mechanistically independent pathways. Lp(a) drives atherogenesis through OxPL-mediated inflammation and antifibrinolytic thrombus potentiation. TRL remnants drive direct subendothelial cholesterol deposition through macrophage uptake. Elevated ApoB reflects a high circulating particle burden that creates sustained exposure to both LDL and the remnant particles driving the TRL pathway. When all three are active simultaneously, the arterial wall is receiving atherogenic insult through three concurrent mechanisms, not one.
Second, the particle populations overlap in risk-amplifying ways. Lp(a) and elevated ApoB are largely independent; having a high Lp(a) does not necessarily mean ApoB is elevated, and vice versa. But when both are present, particle burden includes a disproportionate number of high-risk particles. The 2024 participant-level meta-analysis published in Circulation found that patients with both elevated Lp(a) and elevated LDL-C face up to 90% higher cardiovascular event rates than those with neither (HR 1.90, 95% CI 1.46–2.48). Add an impaired TRL clearance pattern on top of that, and the picture changes further.
The practical consequence of this compounding effect is that a patient with a normal-appearing NHS lipid panel can be carrying a risk profile that is substantially higher than their QRISK3 score suggests. QRISK3 does not include ApoB, Lp(a), or remnant cholesterol in its algorithm. It is calibrated to population averages, not to the precise lipid phenotype of an individual patient with metabolic dysfunction.
Who should be tested, and what the results mean for action
The ESC/EAS 2023 guidelines recommend measuring Lp(a) at least once in every adult's lifetime. The NLA 2024 Focused Update identifies specific populations where the case for testing is most urgent. These include anyone with a first-degree relative who had a heart attack or stroke before the age of 60; anyone with unexplained or premature cardiovascular disease; patients of South Asian or Black African/Caribbean ancestry; patients whose LDL-C is not responding to expected statin therapy; and any adult who is trying to make decisions about preventive intervention.
ApoB is indicated in the same populations, with particular priority for anyone with elevated triglycerides, central adiposity, insulin resistance, PCOS, or fatty liver, where LDL-C discordance is most common and most clinically dangerous.
On the NHS, none of these markers are routinely available. Lp(a) is offered only in limited specialist settings (primarily familial hypercholesterolaemia workup). ApoB is not offered as a standard NHS test. Private advanced lipid testing in the UK ranges from around £30–60 for a single Lp(a) measurement to comprehensive panels at £169–795 depending on the scope of additional markers included.
What to do with the results depends on which markers are elevated, and they are not treated the same way.Lp(a), which is largely genetically fixed, becomes a multiplier that demands more aggressive management of everything else you can change: drive LDL-C and non-HDL-C lower than you otherwise would, tighten blood pressure to below 120/80 mmHg, optimise glucose and insulin resistance, and treat smoking as non-negotiable. An elevated Lp(a) justifies earlier coronary artery calcium scoring and, where appropriate, consideration of PCSK9 inhibitors, not because they are specific to Lp(a), but because they reduce overall atherogenic particle burden while achieving ~25% Lp(a) reduction as a secondary effect. ApoB responds well to dietary fat quality changes, body composition improvement, soluble fibre, sustained exercise, and where indicated statins, ezetimibe, or PCSK9 inhibitors. Triglycerides are the most immediately lifestyle-responsive of the three, and the most important to move first, because normalising them simultaneously reduces ApoB through the VLDL-to-small-dense-LDL cascade.
The clinical approach: one size does not fit all three markers
The biggest clinical mistake when managing this triple pattern is treating Lp(a), ApoB, and triglycerides identically. They have fundamentally different degrees of modifiability through lifestyle, and misunderstanding this leads either to unrealistic expectations for patients with genetic Lp(a) elevation, or to under-treatment of patients whose ApoB and triglycerides are actually highly responsive to well-targeted intervention. The honest clinical picture, marker by marker, is as follows.
Lp(a): the genetically stubborn one. Change everything around it.
With Lp(a) 70–90% genetically determined, lifestyle has a hard ceiling on what it can achieve. A low-carbohydrate dietary pattern may reduce Lp(a) by approximately 10–15%. A whole-food plant-based diet following the Portfolio Diet model, including nuts, legumes, oats, berries, and twelve or more servings of fruit and vegetables daily, has shown approximately 16% reduction within four weeks in some studies. Amla (Indian gooseberry) has been reported in some trials to reduce Lp(a) by around 20%, though industry funding in this area warrants caution about the evidence quality. Exercise and general lifestyle changes have no reliable direct effect on Lp(a) itself.
Lipoprotein apheresis, a process analogous to dialysis applied to blood lipoproteins, can reduce Lp(a) by 60–75% per session and 25–40% with sustained bi-weekly treatment. It is currently the only method that substantially lowers Lp(a), but it is costly, has limited NHS availability (primarily for familial hypercholesterolaemia with LDL above 13 mmol/L), and is approved by the FDA and EMA only for Lp(a) above 60 mg/dL in the context of established cardiovascular disease.
A note on statins and Lp(a): statins do not lower Lp(a), and may modestly raise it in some individuals. Many patients assume that being on a statin covers all their lipid-related cardiovascular risk. For the Lp(a) pathway specifically, this is not the case. This is one of the most important pieces of information that patients with elevated Lp(a) are rarely given by their GP.
The real clinical strategy for elevated Lp(a) is therefore not to chase the number directly through lifestyle; it is to use the knowledge of elevated Lp(a) as a signal to be more aggressive about every other modifiable risk factor. It functions as a risk multiplier that raises the bar for LDL-C targets, blood pressure targets, and the threshold at which pharmacological support is warranted.
ApoB: moderately responsive, with clear and proven levers
ApoB is the most clinically important metric in a private preventive medicine setting because it captures atherogenic particle burden across all lipoprotein classes, not just LDL. The 2026 ACC/AHA guidelines now specifically endorse ApoB testing to assess residual risk beyond LDL-C, particularly in patients with high triglycerides, insulin resistance, or metabolic syndrome. Targets: below 90 mg/dL for primary prevention, below 70 mg/dL for high-risk patients or established ASCVD.
| Intervention | Mechanism | Magnitude |
|---|---|---|
| Replace saturated fat with unsaturated fat | Upregulates LDL receptors in liver | Moderate |
| Mediterranean / Portfolio diet | Reduces LDL particle production, improves clearance | Moderate–significant |
| Aerobic exercise (consistent) | Lowers VLDL production, improves insulin sensitivity | Moderate |
| Resistance training | Improves muscle glucose disposal, reduces hepatic fat | Moderate |
| Weight loss (even modest, 5–10%) | Reduces hepatic VLDL secretion | Significant |
| Soluble fibre (psyllium, oats, legumes) | Interrupts cholesterol reabsorption in gut | Modest |
| Alcohol reduction | Reduces hepatic fat burden and VLDL production | Significant if relevant |
Triglycerides: the most lifestyle-responsive, and the most important to move first
Triglycerides are the best real-time window into a patient's insulin sensitivity. They are also the most directly modifiable of the three through targeted lifestyle changes, and they are clinically the most important to normalise first, because the metabolic dysfunction that drives high triglycerides (VLDL overproduction, impaired clearance) is the same process that generates the small, dense, high-particle-count LDL that elevates ApoB. Fix the upstream metabolic problem and ApoB often improves substantially as a downstream consequence.
- Reduce refined carbohydrates and added sugars: the single most powerful dietary lever. Rapidly absorbed carbohydrates drive hepatic VLDL production directly. This is a first-line, non-pharmacological intervention with results visible within weeks.
- Marine omega-3s (EPA/DHA) at clinical doses: 2–4g/day produces consistent 20–50% triglyceride reduction by reducing hepatic VLDL synthesis and enhancing TRL clearance. This is among the best-evidenced dietary supplement interventions in all of cardiovascular medicine.
- Aerobic exercise: a single bout can lower triglycerides the following day through upregulation of lipoprotein lipase in skeletal muscle; chronic training compounds this effect significantly.
- Alcohol restriction: alcohol acutely and chronically raises hepatic triglyceride production. In private practice patients who drink regularly, this is frequently an under-recognised driver of persistently elevated triglycerides.
- Visceral fat reduction: particularly the reduction of abdominal fat dramatically improves hepatic lipid output and VLDL production. Even a 5% reduction in body weight can lower triglycerides by 20–30%.
- Mediterranean-style eating: emphasising whole grains, vegetables, legumes, nuts, fish, and olive oil addresses the upstream insulin resistance driver of elevated triglyceride-rich lipoproteins.
The clinical priority order when all three are elevated
When a patient presents with all three markers elevated, the order of clinical priority for intervention is: triglycerides first, then ApoB, then Lp(a) third (as a risk context, not a direct target). This is not arbitrary. Triglycerides respond fastest to dietary changes, their elevation signals the insulin resistance that is the root cause driving elevated ApoB, and reducing them substantially often improves ApoB without separate direct intervention. ApoB is then targeted with dietary fat quality, exercise, and body composition work over three to six months, retested to confirm response. Lp(a) is measured once, communicated as a lifetime risk modifier, and used to justify more aggressive targets for everything else, not chased directly with lifestyle.
Validated by the 2026 ACC/AHA guidelines: the updated March 2026 ACC/AHA lipid guidelines specifically endorse Lp(a), ApoB, hsCRP, and triglycerides as a risk-refinement toolkit beyond standard LDL-C. This is precisely the panel that Veridian's Core Metabolic Assessment and Advanced Longevity Assessment, a comprehensive workup that reflects where the evidence has now arrived, even though routine NHS care has not yet caught up.
The emerging pharmacological pipeline for Lp(a), particularly pelacarsen, olpasiran, and muvalaplin, represents the most anticipated development in lipid medicine since PCSK9 inhibitors. Phase 3 trial results are expected between 2025 and 2028. Identifying elevated Lp(a) now means being correctly positioned to access these therapies the moment they receive regulatory approval, rather than discovering the result only after a first cardiovascular event.
The broader message is this: cardiovascular risk is not a single-number problem. The standard cholesterol panel was a necessary simplification for mass-population screening. For individuals who want to understand and actively manage their own vascular biology, three of the most important risk pathways are currently invisible in routine NHS care. Measuring them does not create anxiety. It creates clarity, and in most cases a clear, sequenced, and entirely actionable plan.
Measure all three: Lp(a), ApoB, and triglycerides
Veridian's Core Metabolic Assessment includes the complete triple-threat panel alongside fasting insulin, HbA1c, full thyroid, sex hormones, and inflammatory markers, reviewed in detail with Dr Taiwo.
You will leave with your Lp(a) level (reported in nmol/L, not the ambiguous mg/L scale used by most NHS labs), your ApoB with an evidence-based target, your triglyceride burden in fasting and clinical context, and a personalised plan that sequences interventions in the right order for your specific pattern.
- Lipoprotein(a) is genetically determined, affects 1 in 5 people, and is not measured on the NHS as part of routine cardiovascular screening.
- ApoB measures atherogenic particle number, the most direct handle on arterial exposure, and is frequently elevated even when LDL-C looks normal.
- Triglyceride-rich remnant particles are directly atherogenic and are the most lifestyle-responsive of the three; normalising them first often improves ApoB as a downstream consequence.
- When all three pathways are active simultaneously, risk compounds. The clinical priority order is: triglycerides → ApoB → use Lp(a) to justify tighter targets elsewhere.
- The 2026 ACC/AHA guidelines now explicitly endorse this panel, comprising Lp(a), ApoB, hsCRP, and triglycerides, as the standard risk-refinement toolkit beyond LDL-C.
- Private advanced lipid testing in the UK is the only practical way most adults will access this information before a cardiovascular event makes it urgent.
Related reading: ApoB vs LDL: why particle count matters more than cholesterol content · Fasting insulin and early metabolic dysfunction · Full biomarker guide